Data Exchange Standards in Healthcare
Data exchange standards in healthcare have become the backbone of modern medical systems. These standards define how patient information moves between hospitals, labs, pharmacies, insurers, and patients themselves. Without widely adopted standards, healthcare data remains trapped in silos, leading to duplicated tests, medication errors, and delayed care.
Here, we’ll highlight the major data exchange standards in healthcare in use today, their real-world impact, and emerging developments.
Why Data Exchange Standards in Healthcare Matter?
The U.S. healthcare system alone generates over 2 zettabytes of data annually, yet much of this information historically stayed locked inside proprietary systems. A widely cited 2019 review titled “Waste in the US Health Care System: Estimated Costs and Potential for Savings” estimated total annual waste in U.S. health care at US$760–935 billion, covering multiple waste domains like overtreatment, administrative complexity, care coordination failures, and pricing failures.
However, standardized data exchange reduces administrative burden, improves clinical decision-making, and enables population health management. When a patient visits an emergency department in another state, clinicians can immediately access vaccination records, allergy lists, and recent lab results only because data exchange standards in healthcare exist.
HL7: The Long-Standing Foundation
Health Level Seven (HL7) remains the most recognized name among data exchange standards in healthcare. Founded in 1987, HL7 International develops frameworks for the exchange, integration, sharing, and retrieval of electronic health information.
HL7 Version 2 (v2)
Still the most widely implemented standard globally, HL7 v2 messages handle admissions, discharges, transfers (ADT), orders, and results. Estimates suggest over 90% of U.S. hospitals continue to use HL7 v2 for internal messaging. Its flexibility explains its longevity, though that same flexibility creates variability in implementations.
HL7 Version 3 and CDA
HL7 v3 aimed to solve v2 inconsistencies with a rigorous Reference Information Model (RIM). However, adoption remained limited due to complexity. Likewise, the Clinical Document Architecture (CDA), built on v3 principles, achieved greater success. Consolidated CDA (C-CDA) documents now serve as the standard format for continuity of care documents (CCD) in the United States.
FHIR: The Modern Standard
Fast Healthcare Interoperability Resources (FHIR, pronounced “fire”) has rapidly become the dominant force among current data exchange standards in healthcare. Released in 2014 and reaching maturity with FHIR R4 in 2019 and R5 in 2023, FHIR combines the best features of earlier standards with modern web technologies.
FHIR uses RESTful APIs, JSON and XML formats, and discrete resources (Patient, Observation, MedicationRequest, etc.) that mirror how developers build contemporary applications.
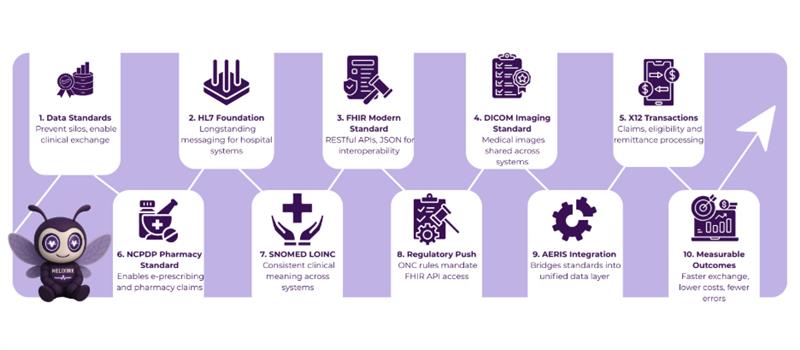
Key Data Exchange Standards in Healthcare Beyond HL7
While FHIR leads new development, several other standards remain critical.
DICOM (Digital Imaging and Communications in Medicine)
DICOM governs medical imaging exchange. Essentially all modern PACS (Picture Archiving and Communication Systems) and modalities (CT, MRI, ultrasound) use DICOM. Recent DICOMweb extensions bring RESTful access to imaging studies, aligning with FHIR initiatives.
X12 for Administrative Transactions
EDI X12 standards (5010 series) handle claims submission (837), eligibility inquiries (270/271), remittance advice (835), and other administrative transactions required under HIPAA. Despite age, X12 transactions still process trillions of dollars annually.
NCPDP for Pharmacy
The National Council for Prescription Drug Programs (NCPDP) SCRIPT standard supports electronic prescribing, while the Telecommunication Standard handles pharmacy claims. Version D.0 has been required since 2019, with ongoing updates for real-time prescription benefit checks.
SNOMED CT and LOINC for Clinical Terminology
These terminologies work alongside transport standards:
- SNOMED CT provides comprehensive clinical terminology (over 350,000 concepts)
- LOINC codes laboratory observations and clinical measurements
Proper use of SNOMED CT and LOINC enables systems to interpret meaning consistently.
U.S. Regulatory Framework Driving Adoption
The federal government has progressively strengthened requirements for data exchange standards in healthcare.
- ONC Cures Act Final Rule (2020) mandates USCDI (United States Core Data for Interoperability) and FHIR-based API access without special effort.
- CMS requires hospitals to send ADT notifications using standardized formats.
- Information blocking provisions impose penalties up to $1 million per violation for withholding data.
AERIS by Helixbeat: Bringing Data Exchange Standards in Healthcare to Life
At Helixbeat, we developed AERIS to solve the everyday challenges of modern healthcare—data overload, interoperability issues, and administrative bottlenecks. Whether it’s a local clinic or a large hospital network, AERIS adapts effortlessly to each environment.
- Seamless Integration: Works with existing EHRs and legacy systems without disrupting ongoing operations.
- Real-Time Collaboration: Connects doctors, labs, pharmacies, and insurers for instant data exchange and decision-making.
- Data Accuracy: Automated workflows and validation tools minimize manual errors, improving the quality of clinical insights.
- Scalability: Grows with your organization as patient volumes and data complexity increase.
- Security & Compliance: Built with HIPAA-grade encryption and audit controls to keep sensitive information protected at all times.
The AERIS Impact in Numbers
Metric | Before AERIS | After AERIS | Outcome |
Data Exchange Speed | Frequent delays | 50% faster exchange | Quicker care delivery |
ROI | Slow recovery | Doubled ROI rate | Greater financial performance |
Operational Costs | High redundancies | Reduced by 30% | Efficient resource use |
Manual Errors | Up to 20% | Decreased by 90% | Accurate patient records |
Your Benefits, Amplified
- 50% Fewer Delays: Real-time data means critical information is always at your fingertips, turning hours into seconds.
- 100% Faster ROI: Plug-and-play integration maximizes your investment without expensive system replacements.
- 30% Cost Savings, 90% Fewer Errors: Automation eliminates waste, saving resources and ensuring accuracy.
How AERIS Works: Your 3-Step Path to Success?
- Connect Seamlessly: Integrate AERIS effortlessly into your existing systems, from legacy EHRs to modern platforms.
- Share Securely: Activate real-time data exchange with HIPAA-compliant encryption. Watch your teams and partners collaborate effortlessly.
- Optimize and Grow: Because AERIS evolves with your organization, it’s set up to help you succeed for the long haul.
How AERIS Works: Your 3-Step Path to Success
- Connect Seamlessly: Integrate AERIS effortlessly into your existing systems, from legacy EHRs to modern platforms.
- Share Securely: Activate real-time data exchange with HIPAA-compliant encryption. Watch your teams and partners collaborate effortlessly.
- Optimize and Grow: Because AERIS evolves with your organization, it’s set up to help you succeed for the long haul.
What Users Say About AERIS
Dr. Sarah L.
Hospital Administrator
John T.
Telemedicine Provider
Emily P.
Healthcare Executive
FAQs
1. What are healthcare data exchange standards?
Healthcare data exchange standards are frameworks that define how medical data is formatted, shared, and interpreted between different healthcare systems and applications.
2. Why are data exchange standards important for clinics and hospitals?
They support smooth communication between systems, reduce manual work, cut duplication, and help providers access accurate patient information at the right time.
3. What is HL7 and how is it used in healthcare?
HL7 is a widely used standard for exchanging clinical and administrative data between hospital systems such as EHRs, labs, and billing platforms.
4. How does AERIS help with interoperability?
AERIS uses industry-trusted standards like HL7 and FHIR to connect EHRs, labs, imaging centers, pharmacies, and insurance systems through real-time, secure data exchange.
Final Thoughts
Data exchange standards in healthcare form the backbone of modern clinical communication, shaping how patient information flows across hospitals, laboratories, pharmacies, and insurers. As the industry continues shifting toward digital-first care models, standards like HL7, FHIR, and others will play a key role in reducing fragmentation and supporting accurate, timely decision-making.
With regulations like the ONC Cures Act and USCDI strengthening nationwide interoperability, healthcare organizations are under growing pressure to adopt systems that support fast, secure, and standardized data exchange. This is where platforms like AERIS make a meaningful difference. By combining trusted data standards with real-time integration, AERIS helps providers overcome legacy barriers, streamline operations, and deliver coordinated care without the usual bottlenecks.


