Clinical Data Integration
Get Started with a Free Demo
New Keyword Page
New Keyword Page
"*" indicates required fields
Clinical data integration combines data from diverse sources like electronic health records (EHRs), laboratory results, imaging systems, and wearable devices. As healthcare generates vast amounts of data, clinical data integration addresses the issue where nearly half of this information goes underutilized in decision-making. By breaking down silos, it gives providers a complete picture, which helps drive progress in both personalized medicine and operational workflows.
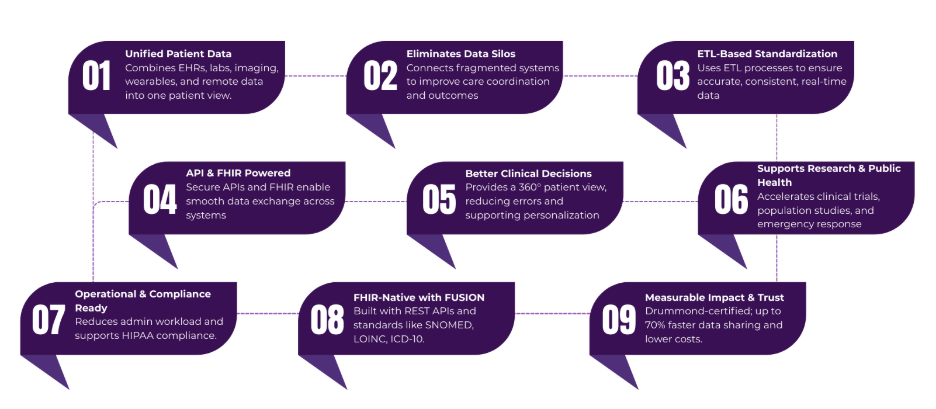
What Is Clinical Data Integration?
Clinical data integration refers to the aggregation and harmonization of clinical data from multiple sources into a single, unified format. This includes patient histories, diagnostic tests, treatment records, and genomic information, often scattered across disparate systems like EHRs, clinical trial databases, and remote monitoring tools. Unlike broader healthcare data integration, which encompasses administrative and financial elements, clinical data integration focuses specifically on patient-centered data to enhance direct care delivery and research.
At its core, this integration involves extracting, transforming, and loading (ETL) data while adhering to standards for compatibility. For example, it bridges the gap between hospitals and outpatient centers, making it easy for staff to pull up live updates on a patient’s health. Technologies like application programming interfaces (APIs) facilitate this by enabling secure data sharing without disrupting existing infrastructures. In clinical trials, it aggregates data from wearables and lab reports to accelerate analysis, reducing manual efforts and minimizing errors.
The process begins with identifying data sources, followed by mapping and standardizing formats to create a single source of truth. This unified dataset supports advanced analytics, like predictive modeling for disease outbreaks or personalized treatment plans. As healthcare shifts toward value-based care, clinical data integration becomes indispensable for maintaining accuracy and timeliness in patient management.
The Importance of Clinical Data Integration in Modern Healthcare
Integrating clinical data is one of the most effective ways to manage the intricacies of healthcare today. With the explosion of data from IoT devices and telemedicine, it bridges gaps that hinder effective care. Providers often face silos where critical information remains isolated. Integration mitigates these issues by offering a 360-degree patient view, which is important for coordinated care across specialties.
In research settings, clinical data integration accelerates discoveries by combining anonymized records for large-scale studies on disease patterns and treatment efficacy. For example, during public health crises like pandemics, real-time integrated data enables rapid resource allocation and surveillance. Regulatory bodies emphasize this importance, with over 80% of organizations adopting standards like HL7 for messaging and FHIR for API-based exchanges to promote interoperability.
Moreover, it supports personalized medicine by incorporating patient-generated data from wearables, so doctors can adjust treatments based on real-time trends. As telemedicine expands in fields like mental health and cardiology, clinical data integration maintains continuity, making it important for sustainable healthcare models.
Key Benefits of Clinical Data Integration
Clinical data integration offers a ton of benefits that make healthcare delivery smoother and more efficient. One big advantage is that doctors can make better choices when they have a complete picture of a patient’s health. By consolidating EHRs, lab results, and imaging, providers gain immediate access to complete histories, which reduces diagnostic errors and supports personalized treatments.
Another important gain involves enhanced operational processes. By streamlining workflows and cutting down on paperwork, clinical data integration frees up staff to focus on patients instead of administrative work. Regulatory compliance and reporting also improve, as unified data facilitates adherence to standards like HIPAA.
Patient experience sees marked enhancement, with integrated portals providing seamless access to records. In clinical research, it speeds up trials by aggregating diverse datasets, leading to faster insights into drug efficacy and population health trends. Overall, these benefits contribute to better outcomes, with 25% of clinicians noting improved decision-making from cohesive data access.
Best Practices for Successful Clinical Data Integration
To achieve effective clinical data integration, organizations should map all data sources, including ownership and dependencies, to identify integration points. Designing scalable architectures with microservices accommodates growth without performance dips. Therefore, adopting standards like FHIR promotes compatibility, and that’s where FUSION comes in.
Unlock Seamless Healthcare Interoperability with FUSION
Imagine a platform that not only meets modern healthcare standards like FHIR but actually pushes your operations forward. That’s FUSION: the FHIR server designed to make interoperability effortless and impactful. Whether you’re a hospital administrator streamlining workflows or a payer optimizing reimbursements, FUSION bridges the gap.
Built on FHIR, it leverages RESTful APIs for plug-and-play integration, enabling seamless connectivity with legacy systems, modern EHRs, and emerging tools like wearable devices and telehealth platforms. This isn’t just compliance, it’s acceleration.
FUSION goes deeper by embedding critical medical coding systems like SNOMED CT, LOINC, and ICD-10 directly into its architecture. This built-in intelligence maintains data consistency and accuracy, transforming raw information into actionable insights ready for clinical decisions, regulatory reporting, and advanced analytics. No more wrestling with mismatched formats or manual mappings: FUSION handles the heavy lifting!
Organizations using FUSION report up to 70% faster data sharing, slashing referral delays by 60% and reducing redundant tests by 25%. That’s not hype; it’s a measurable impact, with providers saving $1,000–$2,000 per patient annually through streamlined claims and operations.
How FUSION Ignites Data-Driven Innovation
The true magic of healthcare FHIR lies in its potential to fuel innovation, and FUSION amplifies this like no other. As a reliable engine for standardized data flows, it powers downstream applications that were once out of reach.
Take chronic disease management, for example. By integrating real-time data from wearables and EHRs, FUSION enables continuous monitoring and proactive interventions, potentially cutting hospital readmissions and optimizing therapies. Or, imagine a telehealth consultation that’s instantly better because the doctor has the patient’s full history right there. FUSION makes that happen, giving virtual care a huge boost in quality and making patients much happier.
Certified Excellence
FUSION is officially certified by the Drummond Group for FHIR-based interoperability, validating its conformance with healthcare data exchange standards HL7, FHIR, and SMART on FHIR. This certification demonstrates that FUSION meets industry-recognized benchmarks for secure, standardized data exchange — giving you the confidence to integrate seamlessly across systems.
What This Means for You
In a complex healthcare ecosystem, FUSION simplifies connectivity and safeguards data integrity. With enterprise-grade uptime (99.99%) and secure authentication powered by OAuth2 and encrypted endpoints, it supports trusted, real-time collaboration between hospitals, labs, and payers.
Whether you’re mapping USCDI elements for regulatory reporting or automating data flows for public-health initiatives, FUSION keeps you compliant with current interoperability frameworks and ready for future mandates.
Final Thoughts
Clinical data integration is a necessity for modern healthcare. By breaking down data silos and unifying patient information from EHRs, labs, imaging, and wearables, providers can deliver faster, safer, and more personalized care. FUSION makes the whole process easy by handling interoperability and compliance for you, giving you useful insights without the stress of manual data mapping.
Ready to transform your data into better patient outcomes? Experience seamless interoperability and intelligent data integration with FUSION.
Frequently Ask Questions
1. Why is health information exchange important in healthcare?
It improves care coordination, reduces duplicate tests, minimizes errors, and helps providers make timely, data-driven decisions across different healthcare settings.
2. What are the main models of health information exchange?
3. Which standards guide health information exchange?
Standards like FHIR and HL7 define consistent data formats, making it easier for EHRs, HIEs, and other healthcare platforms to exchange information.
4. What are the benefits of using health information exchange?
HIE improves care coordination, reduces healthcare costs, supports population health management, enhances research, and increases operational efficiency.
5. How does AERIS enhance healthcare information exchange?
AERIS leverages FHIR standards, connects legacy systems, automates workflows, reduces manual errors, and provides real-time access to patient records and lab results.
1. Why is clinical data integration important?
It eliminates silos, provides a 360-degree patient view, improves care coordination, reduces errors, and accelerates research and personalized treatment.
2. How does FUSION support interoperability?
FUSION uses FHIR-based RESTful APIs to connect legacy systems, modern EHRs, wearables, and telehealth platforms seamlessly.
3. What standards does FUSION comply with?
FUSION supports HL7, FHIR, SMART on FHIR, and includes embedded coding systems like SNOMED CT, LOINC, and ICD-10 for consistent data handling.
4. Can FUSION integrate wearable and telehealth data?
Yes. FUSION can ingest real-time data from wearable devices and telehealth platforms, facilitating continuous monitoring and proactive care.


