Data Interoperability in Healthcare
Get Started with a Free Demo
New Keyword Page
New Keyword Page
"*" indicates required fields
Data interoperability in healthcare stands as a foundational element in modern medical systems. This process facilitates the secure access and integration of electronic health records (EHRs) across various platforms. Without effective data interoperability in healthcare, providers often face repeated tests, potential errors, and increased expenses. Therefore, government bodies like the Office of the National Coordinator for Health Information Technology (ONC) lead efforts to standardize this exchange.
Here, we explore the core concepts, standards, benefits, challenges, and emerging trends in data interoperability in healthcare.
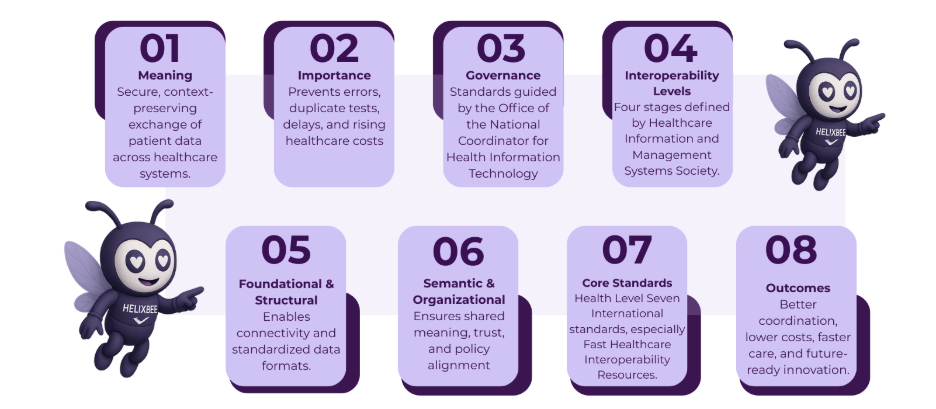
Understanding Data Interoperability in Healthcare
Data interoperability in healthcare involves the capability of disparate systems, like EHRs, lab systems, imaging devices, and wearable technologies, to exchange and interpret health information without loss of meaning or context. The Healthcare Information and Management Systems Society (HIMSS) outlines four progressive levels of interoperability: foundational, structural, semantic, and organizational.
Foundational interoperability establishes basic connectivity, where one system sends data to another, similar to opening channels for information flow. Structural interoperability, also called syntactic, focuses on formatting data consistently so that receiving systems can parse it correctly. Standards like Consolidated Clinical Document Architecture (C-CDA) and direct messaging protocols maintain this uniformity.
Semantic interoperability advances further by enabling systems not only to receive data but also to understand and apply it accurately. This requires standardized vocabularies and codes, addressing issues where varied terminologies in scattered systems create confusion. Therefore, regulations like the Health Data, Technology, and Interoperability: Certification Program Updates, Algorithm Transparency, and Information Sharing (HTI-1) rule mandate FHIR-enabled APIs and the sharing of key data elements through the United States Core Data for Interoperability (USCDI).
Organizational interoperability integrates all previous levels with governance, policies, and trust mechanisms across entities. Initiatives like the Trusted Exchange Framework and Common Agreement (TEFCA) promote secure exchanges by emphasizing privacy and data stewardship. These levels collectively enable comprehensive data sharing, though progress varies, with larger organizations achieving higher maturity compared to rural or smaller providers.
Standards and Technologies Driving Data Interoperability in Healthcare
Several standards form the backbone of data interoperability in healthcare, providing frameworks for consistent exchange. Health Level Seven International (HL7) standards, including FHIR, specify data types, codes, and terminologies for accurate transmission. FHIR, an open-source framework, organizes information into resources like patient demographics, conditions, and medications, facilitating movement between systems.
The USCDI standardizes health data classes like clinical notes, allergies, lab results, and medications for nationwide exchange. Digital Imaging and Communications in Medicine (DICOM) handles medical imaging, while Systematized Nomenclature of Medicine – Clinical Terms (SNOMED CT) and Logical Observation Identifiers Names and Codes (LOINC) provide terminologies for clinical findings and lab observations.
Additionally, the Centers for Medicare & Medicaid Services (CMS) Interoperability Framework promotes FHIR APIs, machine-readable formats, and timely responses by 2026, including clinical documents and appointment notifications. These technologies maintain compatibility, openness, and security in data flows.
Benefits of Data Interoperability in Healthcare
Implementing data interoperability in healthcare yields multiple advantages. Firstly, it simplifies how teams coordinate, which ultimately leads to better results for the patient. Providers gain easier access to complete histories, reducing redundant tests, drug interactions, and communication gaps. This leads to faster emergency responses and better management of chronic conditions through shared insights among teams, patients, and payers.
Cost savings is another key benefit. Having systems that work together makes it simple to see what’s happening in the data, so you can fix performance issues and use your resources more wisely. Additionally, patient experiences improve through reduced paperwork and empowered self-management, as individuals access their data via apps. Overall, these benefits contribute to safer, more efficient healthcare ecosystems.
Unlock Seamless Healthcare Data Interoperability with FUSION
Imagine a platform that not only meets modern healthcare standards like FHIR but actually pushes your operations forward. That’s FUSION: the FHIR server designed to make interoperability effortless and impactful. Whether you’re a hospital administrator streamlining workflows or a payer optimizing reimbursements, FUSION bridges the gap.
Built on FHIR, it leverages RESTful APIs for plug-and-play integration, enabling seamless connectivity with legacy systems, modern EHRs, and emerging tools like wearable devices and telehealth platforms. This isn’t just compliance, it’s acceleration.
FUSION goes deeper by embedding critical medical coding systems like SNOMED CT, LOINC, and ICD-10 directly into its architecture. This built-in intelligence maintains data consistency and accuracy, transforming raw information into actionable insights ready for clinical decisions, regulatory reporting, and advanced analytics. No more wrestling with mismatched formats or manual mappings: FUSION handles the heavy lifting!
Organizations using FUSION report up to 70% faster data sharing, slashing referral delays by 60% and reducing redundant tests by 25%. That’s not hype; it’s a measurable impact, with providers saving $1,000–$2,000 per patient annually through streamlined claims and operations.
How FUSION Ignites Data-Driven Innovation?
The true magic of healthcare FHIR lies in its potential to fuel innovation, and FUSION amplifies this like no other. As a reliable engine for standardized data flows, it powers downstream applications that were once out of reach.
Take chronic disease management, for example. By integrating real-time data from wearables and EHRs, FUSION enables continuous monitoring and proactive interventions, potentially cutting hospital readmissions and optimizing therapies. Or, imagine a telehealth consultation that’s instantly better because the doctor has the patient’s full history right there. FUSION makes that happen, giving virtual care a huge boost in quality and making patients much happier.
Certified Excellence
FUSION is officially certified by the Drummond Group for FHIR-based interoperability, validating its conformance with healthcare data exchange standards HL7, FHIR, and SMART on FHIR. This certification demonstrates that FUSION meets industry-recognized benchmarks for secure, standardized data exchange — giving you the confidence to integrate seamlessly across systems.
What This Means for You?
In a complex healthcare ecosystem, FUSION simplifies connectivity and safeguards data integrity. With enterprise-grade uptime (99.99%) and secure authentication powered by OAuth2 and encrypted endpoints, it supports trusted, real-time collaboration between hospitals, labs, and payers.
Whether you’re mapping USCDI elements for regulatory reporting or automating data flows for public-health initiatives, FUSION keeps you compliant with current interoperability frameworks and ready for future mandates.
Final Thoughts
Looking ahead to 2026 and beyond, data interoperability in healthcare will integrate artificial intelligence (AI) to automate exchanges and derive insights. Deeper FHIR adoption, alongside event-driven data flows, will incorporate social determinants of health (SDoH) and behavioral data. Cloud-based solutions and global expansions will enhance population management, with AI aiding predictive analytics. Regulatory pushes, like TEFCA expansions, will drive compliance and innovation.
By addressing current hurdles and embracing new technologies like FUSION, the sector can achieve greater equity and quality in care delivery.
Frequently Ask Questions
What is data interoperability in healthcare?
Data interoperability in healthcare refers to the ability of different health information systems to exchange, interpret, and use data accurately across platforms without losing meaning or context.
Why is data interoperability important for healthcare providers?
It reduces duplicate tests, minimizes medical errors, improves care coordination, lowers operational costs, and gives providers access to complete patient histories in real time.
What are the four levels of healthcare data interoperability?
The four levels defined by HIMSS are foundational, structural, semantic, and organizational interoperability, each representing increasing maturity in data exchange and usability.
How does FUSION help organizations achieve interoperability?
FUSION provides a FHIR-based server with built-in clinical coding standards, secure APIs, and plug-and-play integration that simplifies data exchange across systems.


