EHR EMR Interoperability with FUSION
Get Started with a Free Demo
New Keyword Page
New Keyword Page
"*" indicates required fields
Today, EHR/EMR interoperability stands as a cornerstone for modern medical practices. It refers to the ability of Electronic Health Records (EHR) and Electronic Medical Records (EMR) systems to communicate, exchange, and interpret shared data effectively. As healthcare providers increasingly rely on digital tools, achieving robust EHR/EMR interoperability becomes important for delivering coordinated care.
In this blog, we discuss the fundamentals, standards, benefits, and solutions of EHR/EMR interoperability.
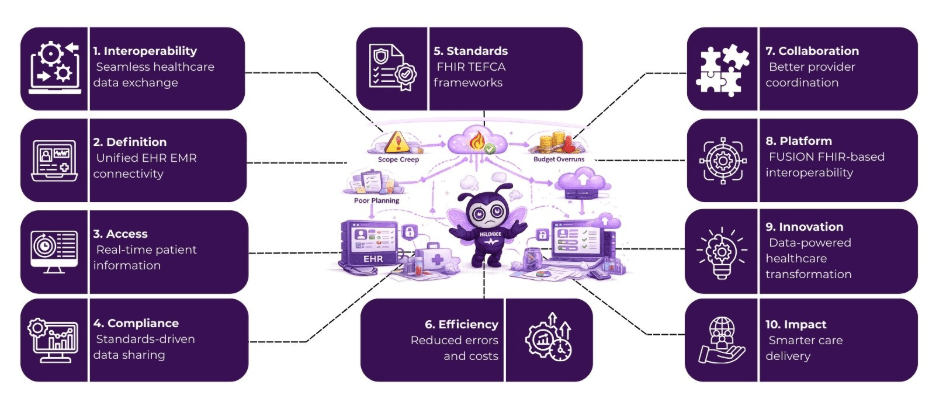
What is EHR/EMR Interoperability?
EHR/EMR interoperability involves the seamless integration of health information systems, so data can flow between different platforms without losing meaning or context. EHR systems typically involve a broader scope, including patient history across multiple providers, while EMRs focus on records within a single practice. However, the terms are often used interchangeably in discussions about data exchange.
At its core, EHR/EMR interoperability enables healthcare professionals to access complete patient information in real time, regardless of the originating system. This capability aligns with the goals of value-based care models, where outcomes depend on comprehensive data availability. As of 2025, foundational EHR/EMR interoperability is widespread across many healthcare organizations globally, but semantic levels remain less common.
Regulatory frameworks, like the 21st Century Cures Act, mandate information sharing, creating conditions that promote EHR/EMR interoperability.
Key Standards Driving EHR/EMR Interoperability
Standards form the backbone of EHR/EMR interoperability. The most prominent is Fast Healthcare Interoperability Resources (FHIR), developed by Health Level Seven International (HL7). FHIR uses modern web technologies like RESTful APIs to enable flexible, modular data sharing.
Another critical framework is the Trusted Exchange Framework and Common Agreement (TEFCA), launched by ONC. TEFCA encourages nationwide health information sharing by connecting QHINs into a single, secure “network of networks”. The CMS Interoperability Framework, unveiled in July 2025, introduces voluntary standards for data access, with early adopters aiming for full adoption by mid-2026.
Additional standards include ICD-10 for coding consistency and DICOM for imaging.
Benefits of EHR/EMR Interoperability
EHR/EMR interoperability yields significant advantages for patients, providers, and systems. First, it enhances patient-centered care by providing comprehensive views of medical histories. Studies show that interoperable systems reduce medication safety incidents ranging from about 15% up to over 50%.
Cost reductions represent another key benefit. By automating redundant processes, like manual data entry, healthcare facilities lower operational expenses. Research indicates that organizations with advanced EHR/EMR interoperability save on average 15% in administrative costs through efficient coordination.
Thirdly, improved communication among providers boosts collaboration, especially in complex cases involving multiple specialists. For patients, this translates to faster access to records via apps. In terms of public health, interoperable data supports population health analytics.
Safety improvements are evident too. Integrated systems decreased hospital readmissions by facilitating timely information sharing.
Unlock Seamless EHR/EMR Interoperability with FUSION
Imagine a platform that not only meets modern healthcare standards like FHIR but actually pushes your operations forward. That’s FUSION: the FHIR server designed to make interoperability effortless and impactful. Whether you’re a hospital administrator streamlining workflows or a payer optimizing reimbursements, FUSION bridges the gap.
Built on FHIR, it leverages RESTful APIs for plug-and-play integration, enabling seamless connectivity with legacy systems, modern EHRs, and emerging tools like wearable devices and telehealth platforms. This isn’t just compliance, it’s acceleration.
FUSION goes deeper by embedding critical medical coding systems like SNOMED CT, LOINC, and ICD-10 directly into its architecture. This built-in intelligence maintains data consistency and accuracy, transforming raw information into actionable insights ready for clinical decisions, regulatory reporting, and advanced analytics. No more wrestling with mismatched formats or manual mappings: FUSION handles the heavy lifting!
Organizations using FUSION report up to 70% faster data sharing, slashing referral delays by 60% and reducing redundant tests by 25%. That’s not hype; it’s a measurable impact, with providers saving $1,000–$2,000 per patient annually through streamlined claims and operations.
Final Thoughts
EHR/EMR interoperability is central to modern healthcare delivery. By enabling seamless data exchange across providers, systems, and devices, interoperability enhances patient care, reduces costs, and strengthens provider collaboration. Platforms like FUSION take interoperability a step further by leveraging FHIR standards, built-in coding systems, and real-time connectivity to transform healthcare operations.
Take the next step with FUSION today to unify your healthcare systems, optimize workflows, and deliver faster, safer, and more efficient care.
Frequently Ask Questions
1. Why is health information exchange important in healthcare?
It improves care coordination, reduces duplicate tests, minimizes errors, and helps providers make timely, data-driven decisions across different healthcare settings.
2. What are the main models of health information exchange?
3. Which standards guide health information exchange?
Standards like FHIR and HL7 define consistent data formats, making it easier for EHRs, HIEs, and other healthcare platforms to exchange information.
4. What are the benefits of using health information exchange?
HIE improves care coordination, reduces healthcare costs, supports population health management, enhances research, and increases operational efficiency.
5. How does AERIS enhance healthcare information exchange?
AERIS leverages FHIR standards, connects legacy systems, automates workflows, reduces manual errors, and provides real-time access to patient records and lab results.
1. What is EHR/EMR interoperability?
It is the ability of EHR and EMR systems to exchange and interpret healthcare data across different platforms effectively.
2. How does FHIR support interoperability?
FHIR standardizes data structures and uses RESTful APIs to enable flexible, modular, and real-time data sharing between systems.
3. What are the main benefits of EHR/EMR interoperability?
Key benefits include improved patient care, reduced administrative costs, better provider collaboration, and enhanced safety and compliance.
4. Is FUSION scalable for different healthcare organizations?
Yes, FUSION is built to handle hospitals, clinics, and payers of all sizes, supporting growth, heavy data loads, and advanced analytics.


