Healthcare Data Interoperability
Get Started with a Free Demo
New Keyword Page
New Keyword Page
"*" indicates required fields
In a world where medical tech moves fast, we need healthcare systems that actually talk to each other. When healthcare providers and their systems finally speak the same language, it’s the patients who really win. It means everyone on your care team is on the same page, which leads to much better recovery and support.
Here, we’ll discuss the definition, standards, benefits, and future trends of healthcare data interoperability.
What Is Healthcare Data Interoperability?
Healthcare data interoperability refers to the ability of various information systems, devices, and applications to access, exchange, integrate, and cooperatively use data in a coordinated manner. The Healthcare Information and Management Systems Society (HIMSS) defines it as the capacity for systems to work together within and across organizational boundaries to advance effective delivery of healthcare. This goes beyond mere data exchange; it involves interpreting shared information correctly to support clinical decisions.
We can break down healthcare data interoperability into four levels: foundational, structural, semantic, and organizational. Foundational interoperability establishes basic connectivity between systems. Structural interoperability defines the format and syntax of data exchange. Semantic interoperability allows systems to interpret and use the data meaningfully, while organizational interoperability incorporates governance, policy, and legal frameworks for seamless sharing.
For example, when a patient moves from a primary care physician to a specialist, interoperable systems allow the specialist to access the patient’s complete medical history without redundant tests. This process reduces delays and enhances accuracy in diagnosis. The Office of the National Coordinator for Health Information Technology (ONC) emphasizes that interoperability enables clinicians to deliver safe, effective, patient-centered care by providing access to electronic health information.
Standards and Technologies Driving Healthcare Data Interoperability
Several standards facilitate healthcare data interoperability, with Health Level Seven International (HL7) playing an important role. HL7 develops frameworks for exchanging, integrating, sharing, and retrieving electronic health information. The Fast Healthcare Interoperability Resources (FHIR) standard, created by HL7, represents a modern approach to data exchange. FHIR uses modular components called “Resources” as the basic data format, supporting RESTful APIs and formats like JSON for web-based interactions.
FHIR emerged in 2010 as an open standard to overcome limitations of previous HL7 versions, which were often monolithic. It allows for easier integration with mobile apps and cloud services, making it suitable for contemporary healthcare environments. Other standards include Digital Imaging and Communications in Medicine (DICOM) for medical imaging and Consolidated Clinical Document Architecture (CCDA) for document-based exchanges.
The 21st Century Cures Act, enacted in 2016, mandates interoperability by prohibiting information blocking and requiring secure exchange of electronic health information (EHI). The Act defines interoperability as the secure exchange of EHI without special effort from users, promoting the use of APIs for better data access. ONC’s Cures Act Final Rule further supports this by implementing requirements for seamless data access and updating the Health IT Certification Program.
Benefits of Healthcare Data Interoperability
Healthcare data interoperability offers multiple advantages, starting with enhanced patient safety and reduced medical errors. Full access to patient records allows providers to identify allergies, medications, and past treatments promptly, which minimizes risks.
Improved care coordination ranks high among benefits. When data flows freely between providers, patients experience smoother transitions, like from hospital to home care. This holistic view integrates clinical data with social determinants of health (SDOH), leading to comprehensive treatment plans.
Cost savings is another key benefit. By avoiding redundant procedures and streamlining administrative tasks, interoperability reduces healthcare expenditures. Studies indicate that better data sharing lowers costs through efficient utilization and improved quality metrics. Additionally, it empowers patients by granting access to their own data.
Unlock Seamless Healthcare Data Interoperability with FUSION
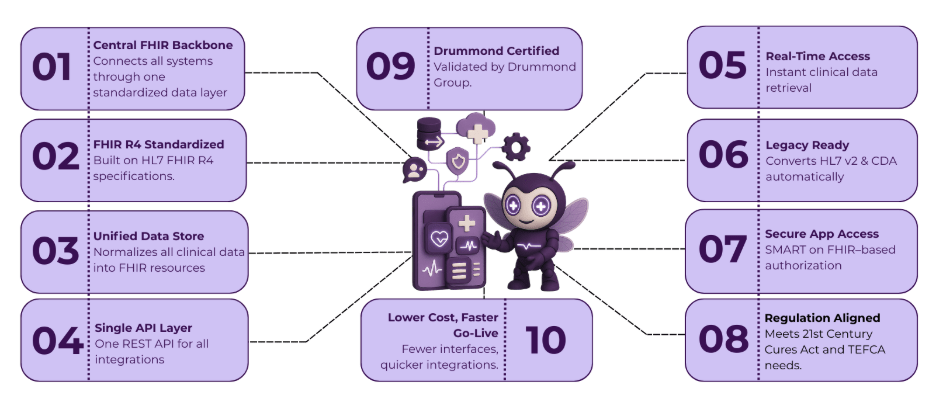
Imagine a platform that not only meets modern healthcare standards like FHIR but actually pushes your operations forward. That’s FUSION: the FHIR server designed to make interoperability effortless and impactful. Whether you’re a hospital administrator streamlining workflows or a payer optimizing reimbursements, FUSION bridges the gap.
Built on FHIR, it leverages RESTful APIs for plug-and-play integration, enabling seamless connectivity with legacy systems, modern EHRs, and emerging tools like wearable devices and telehealth platforms. This isn’t just compliance, it’s acceleration.
FUSION goes deeper by embedding critical medical coding systems like SNOMED CT, LOINC, and ICD-10 directly into its architecture. This built-in intelligence maintains data consistency and accuracy, transforming raw information into actionable insights ready for clinical decisions, regulatory reporting, and advanced analytics. No more wrestling with mismatched formats or manual mappings: FUSION handles the heavy lifting!
Organizations using FUSION report up to 70% faster data sharing, slashing referral delays by 60% and reducing redundant tests by 25%. That’s not hype; it’s a measurable impact, with providers saving $1,000–$2,000 per patient annually through streamlined claims and operations.
How FUSION Ignites Data-Driven Innovation?
The true magic of healthcare FHIR lies in its potential to fuel innovation, and FUSION amplifies this like no other. As a reliable engine for standardized data flows, it powers downstream applications that were once out of reach.
Take chronic disease management, for example. By integrating real-time data from wearables and EHRs, FUSION enables continuous monitoring and proactive interventions, potentially cutting hospital readmissions and optimizing therapies. Or, imagine a telehealth consultation that’s instantly better because the doctor has the patient’s full history right there. FUSION makes that happen, giving virtual care a huge boost in quality and making patients much happier.
Certified Excellence
FUSION is officially certified by the Drummond Group for FHIR-based interoperability, validating its conformance with healthcare data exchange standards HL7, FHIR, and SMART on FHIR. This certification demonstrates that FUSION meets industry-recognized benchmarks for secure, standardized data exchange — giving you the confidence to integrate seamlessly across systems.
What This Means for You
In a complex healthcare ecosystem, FUSION simplifies connectivity and safeguards data integrity. With enterprise-grade uptime (99.99%) and secure authentication powered by OAuth2 and encrypted endpoints, it supports trusted, real-time collaboration between hospitals, labs, and payers.
Whether you’re mapping USCDI elements for regulatory reporting or automating data flows for public-health initiatives, FUSION keeps you compliant with current interoperability frameworks and ready for future mandates.
Future Trends in Healthcare Data Interoperability
Looking ahead, artificial intelligence (AI) integration promises to transform healthcare data interoperability. AI can automate data mapping, predict integration issues, and extract insights from disparate sources, making exchanges more efficient.
Expansion of FHIR adoption will continue, with more systems incorporating APIs for real-time access. Event-driven workflows and cloud-based platforms will enable dynamic data sharing.
Regulatory advancements, such as updates to the Cures Act, will push for broader compliance. As global standards start to align, it’ll be much easier for people to get medical care across borders.
Final Thoughts
Healthcare data interoperability has moved from being a technical ambition to a foundational requirement for modern care delivery. As healthcare systems grow more complex, the ability to exchange and interpret data accurately across platforms directly impacts patient safety, clinical outcomes, operational efficiency, and cost control.
This is where a FHIR server like FUSION makes a tangible difference. By simplifying FHIR-based integration, embedding standardized medical vocabularies, and supporting secure, real-time data exchange, FUSION helps healthcare organizations move beyond basic compliance toward true data-driven care.
Frequently Ask Questions
1. Why is interoperability important in healthcare?
It improves care coordination, reduces medical errors, lowers costs, and provides clinicians with a complete view of patient health information.
2. What are the four levels of healthcare interoperability?
The four levels are foundational, structural, semantic, and organizational interoperability, each representing increasing complexity and value in data exchange.
3. What role does HL7 play in interoperability?
HL7 develops global standards that define how healthcare data is structured, shared, and interpreted across systems.
4. Is FUSION compliant with industry standards?
Yes, FUSION is certified by the Drummond Group and conforms to HL7, FHIR, and SMART on FHIR standards.
5. What future trends will shape healthcare interoperability?
AI-driven data mapping, expanded FHIR adoption, cloud-based platforms, and evolving regulations will define the next phase of interoperable healthcare systems.


