Table of Contents
Introduction
Medical billing is a tricky process. It involves multiple steps, from patient registration to claim submission and payment posting. A single error can result in a denied claim, causing revenue loss and extra administrative work.
If you’re a healthcare provider, you probably know the frustration of dealing with rejected claims. According to the Medical Group Management Association (MGMA), nearly 30% of claim denials happen due to coding errors or missing information. That’s a significant chunk of your revenue tied up in preventable mistakes.
But what if there was an easier way?
Enter Paynova – an advanced medical billing software designed to streamline the claims process, reduce denials, and help healthcare providers maximize their revenue.
Let’s explore the most common challenges in medical billing software and how Paynova helps tackle them efficiently.
The Challenges of Medical Billing and Claim Denials
Medical billing is a complex process involving multiple steps, from patient registration to claim submission and payment posting. Errors at any stage can lead to claim denials, causing revenue loss and administrative burdens. According to the Medical Group Management Association (MGMA), nearly 30% of denied claims are due to coding errors or missing information.
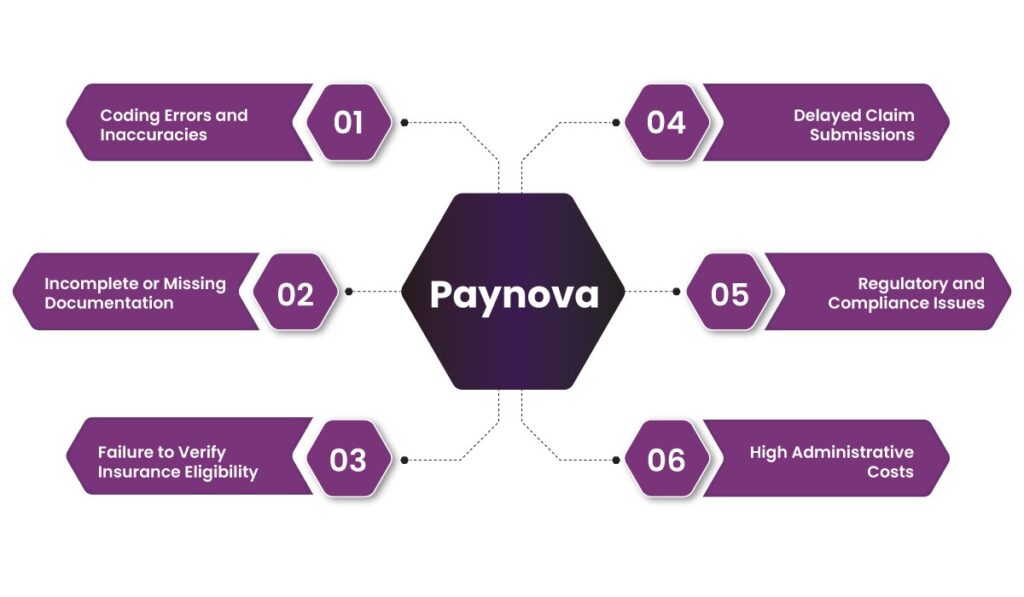
1. Coding Errors and Inaccuracies
Incorrect CPT and ICD-10 codes, mismatched patient demographics, and lack of specificity in diagnosis codes are common issues. For example, using an outdated code for a procedure can lead to automatic rejection.
2. Incomplete or Missing Documentation
Claims require accurate documentation, including physician signatures and supporting medical records. The Healthcare Financial Management Association (HFMA) reports that 21% of denials result from missing documentation.
3. Failure to Verify Insurance Eligibility
Nearly 23% of claims are denied due to expired coverage, incorrect insurance details, or lack of prior authorization. Real-time insurance verification can help prevent these issues.
4. Delayed Claim Submissions
Insurers impose strict filing deadlines, and late submissions lead to revenue loss. The American Academy of Family Physicians (AAFP) estimates that providers lose up to 6% of revenue due to late claims.
5. Regulatory and Compliance Issues
Frequent updates to Medicare, Medicaid, and HIPAA regulations make compliance difficult. In 2023, CMS introduced over 300 billing rule changes, increasing the risk of denials.
6. High Administrative Costs
Manual claims processing is costly, with the Council for Affordable Quality Healthcare (CAQH) estimating $118 billion in annual administrative expenses.
Addressing these challenges requires automation, real-time verification, and proactive denial management to ensure faster reimbursements and improved cash flow.
How Paynova Reduces Claim Denials?
Paynova is a cutting-edge medical billing software designed to tackle common issues in claims processing. By leveraging automation, AI-driven analytics, and real-time verification, Paynova helps healthcare providers reduce denials and improve revenue collection. Here’s how:
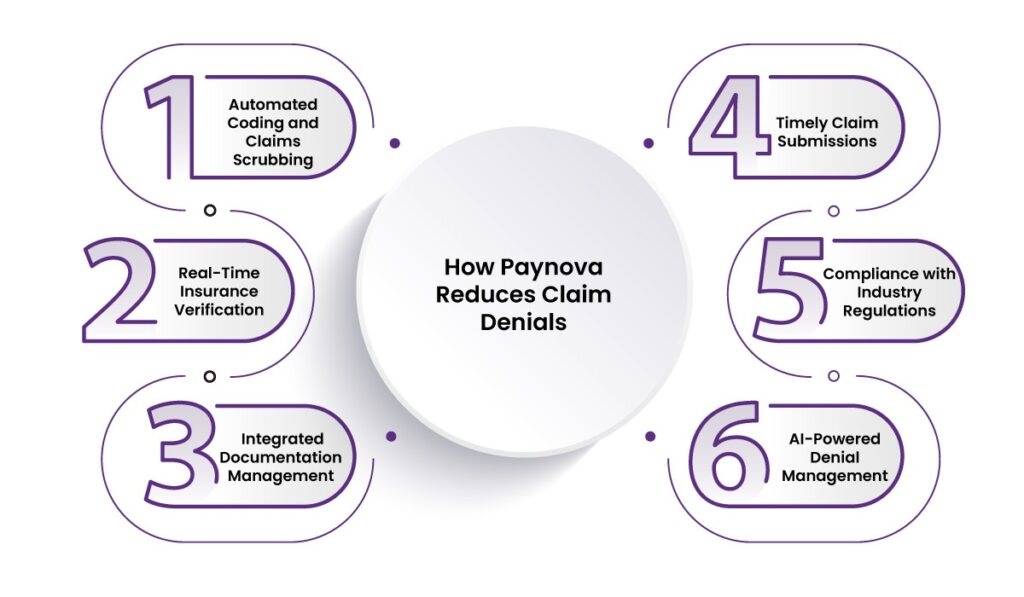
1. Automated Coding and Claims Scrubbing
One of the biggest reasons for claim denials is coding errors. Medical billing involves thousands of CPT, ICD-10, and HCPCS codes, and even a minor mistake can result in rejection. Paynova features an automated coding assistant that verifies these codes before claim submission. It also provides a claim scrubbing feature, which scans for inconsistencies and errors before the claim reaches the payer. This ensures a higher acceptance rate.
Example: A dermatologist submits a claim for a laser skin treatment but accidentally enters an outdated CPT code. Without Paynova, the claim would be denied, leading to delays and resubmission costs. With Paynova, the Medical billing software flags the outdated code and suggests the correct one before submission, ensuring timely reimbursement.
2. Real-Time Insurance Verification
Incorrect or expired insurance details account for nearly 23% of claim denials. Paynova’s real-time insurance eligibility verification allows providers to check patient coverage, policy status, and pre-authorization requirements instantly. This ensures claims are filed with accurate insurance information, reducing the chances of rejection.
Example: A patient visits a cardiologist for a routine checkup, but their insurance coverage changed recently. Without verification, the claim could be denied. Paynova checks the patient’s eligibility in real time, prompting the provider to update records and obtain necessary pre-authorizations before rendering services.
3. Integrated Documentation Management
Many claims are denied due to missing documentation, such as physician notes, lab results, or treatment records. Paynova offers electronic document management, ensuring that all required documents are attached to claims before submission. This not only reduces denials but also speeds up approvals.
Example: A rheumatologist prescribes an expensive biologic drug, but the insurance company requires supporting lab results. With Paynova, the provider can automatically attach relevant test reports, ensuring the claim is processed without additional requests for information.
4. Timely Claim Submissions
Late claim submissions can lead to revenue loss, as insurers have strict filing deadlines. Paynova includes automated reminders and batch claim submission features, helping healthcare providers meet these deadlines and avoid rejections due to tardiness.
Example: A busy orthopedic clinic forgets to submit claims for multiple surgeries performed a month ago. With Paynova, automated reminders notify the billing staff of upcoming deadlines, ensuring claims are submitted promptly and revenue isn’t lost.
5. Compliance with Industry Regulations
Healthcare regulations change frequently, making compliance a challenge. Paynova continuously updates its Medical billing software to comply with Medicare, Medicaid, HIPAA, and payer-specific billing rules. This minimizes compliance-related denials and protects providers from audits and penalties.
Example: A physical therapy practice unknowingly submits claims using an outdated Medicare billing rule. With Paynova, the medical billing software automatically updates billing protocols and alerts the provider, ensuring compliance and preventing claim denials.
6. AI-Powered Denial Management
Paynova’s AI-driven analytics track denial trends, helping providers identify patterns and resolve issues proactively. With real-time insights, providers can fix claim errors before submission, reducing denial rates by 40% or more.
Example: A gastroenterology clinic notices frequent denials related to anesthesia billing. Paynova’s AI highlights the issue and recommends using appropriate modifiers, preventing future denials and improving revenue flow.
How Paynova Boosts Revenue for Healthcare Providers?
Beyond reducing claim denials, Paynova also enhances revenue collection and financial performance. Here’s how:
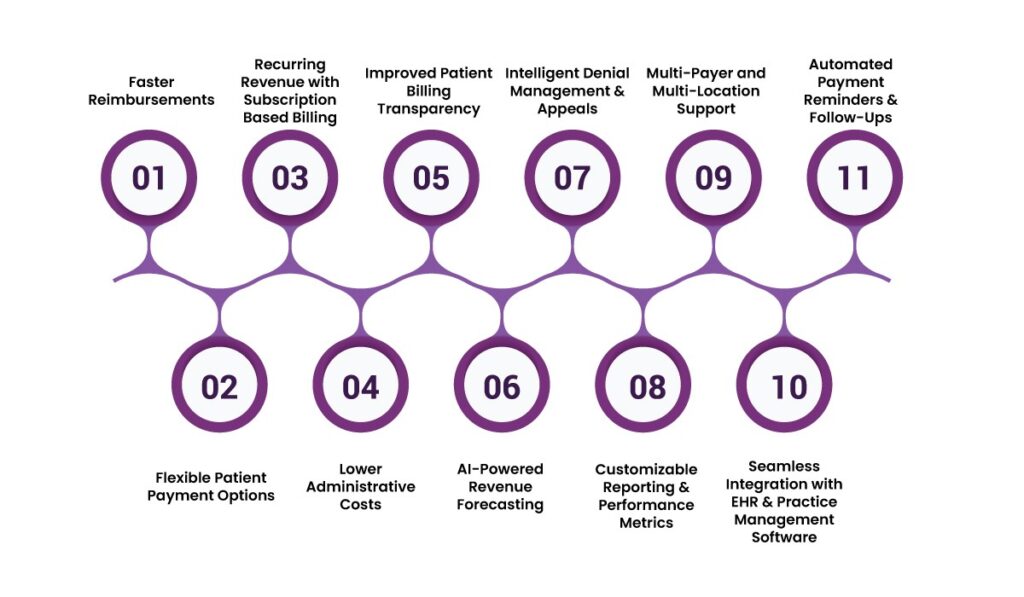
1. Faster Reimbursements
By automating coding, verification, and submission, Paynova accelerates the claims process. Providers receive payments faster, improving cash flow and reducing outstanding receivables.
Example: A mental health clinic using manual billing waits an average of 45 days for claim processing. With Paynova’s automated Medical billing software, claims are submitted accurately and approved within 15 days, improving cash flow.
2. Flexible Patient Payment Options
Patients often struggle with medical bills, leading to delayed payments. Paynova includes online payment portals, digital wallets, and installment plans, allowing patients to pay conveniently. This reduces unpaid bills and improves collection rates.
Example: A dental clinic allows patients to split payments into three installments through Paynova, increasing payment compliance and reducing bad debt.
3. Recurring Revenue with Subscription-Based Billing
For telehealth and concierge medical services, Paynova supports automated monthly billing, ensuring consistent cash flow for providers.
Example: A telemedicine provider offers monthly membership plans. Paynova automates recurring billing, reducing administrative work and ensuring predictable revenue.
4. Lower Administrative Costs
Manual claims processing is expensive and time-consuming. By automating these processes, Paynova reduces staff workload, cutting operational costs and allowing healthcare teams to focus more on patient care.
Example: A small family practice previously required three staff members for billing. With Paynova, automation reduces the need for manual data entry, allowing staff to focus on patient engagement.
5. Improved Patient Billing Transparency
Confusing medical bills often lead to disputes and delayed payments. Paynova provides clear, itemized digital invoices, helping patients understand their charges and pay promptly.
Example: A surgical center using Paynova sends automated invoices with a detailed cost breakdown. Patients appreciate the transparency, leading to faster payments and fewer billing disputes.
6. AI-Powered Revenue Forecasting
Paynova’s AI-driven analytics help healthcare providers predict revenue trends based on claim approvals, patient payments, and payer reimbursements. This allows organizations to make data-driven financial decisions.
Example:
A multi-specialty clinic uses Paynova’s revenue forecasting tool to predict quarterly income based on claim success rates. This helps them optimize staffing, budgeting, and expansion planning.
7. Intelligent Denial Management & Appeals
Even with the best Medical billing software, some claims get denied. Paynova tracks denial patterns, provides instant alerts, and offers automated appeal suggestions, increasing the success rate of re-submitted claims.
Example:
A cardiology clinic had a 20% claim denial rate before using Paynova. After implementing the automated denial management feature, denial rates dropped to 5%, ensuring higher revenue retention.
8. Customizable Reporting & Performance Metrics
Paynova provides real-time financial dashboards that display:
- Claim approval rates
- Patient payment trends
- Denial reasons
- Payer reimbursement speed
This enables healthcare providers to optimize billing workflows and improve revenue collection strategies.
Example:
A hospital uses Paynova’s reporting tools to identify slow-paying insurance providers and adjust follow-up strategies, reducing their accounts receivable period by 25%.
9. Multi-Payer and Multi-Location Support
For hospitals, specialty clinics, and large healthcare networks, Paynova supports multiple payers, facilities, and provider groups, streamlining complex billing operations.
Example:
A dermatology chain with five locations previously had separate medical billing software. Paynova unified their billing, claims, and reporting across all locations, reducing inefficiencies and increasing revenue by 15%.
10. Seamless Integration with EHR & Practice Management Software
Paynova seamlessly integrates with Electronic Health Records (EHR) and Practice Management Systems (PMS), eliminating duplicate data entry and minimizing errors.
Example:
An orthopedic clinic previously had billing discrepancies due to separate EHR and Medical billing software. With Paynova’s EHR integration, claim accuracy improved by 35%, reducing revenue loss.
11. Automated Payment Reminders & Follow-Ups
Late patient payments are a major issue in medical billing. Paynova includes automated payment reminders via SMS, email, and phone, ensuring timely collections.
Example:
A pediatric clinic using Paynova’s automated reminder system saw a 60% reduction in late payments, improving overall revenue stability.
By these methods, Paynova ensures providing revenue cycle to medical providers.
Final words
Paynova is more than just a medical billing software—it’s a comprehensive revenue cycle management solution that optimizes cash flow, reduces denials, improves operational efficiency, and enhances the patient payment experience. By leveraging automation, AI-powered analytics, and seamless integrations, Paynova empowers healthcare providers to focus on patient care while ensuring a steady and predictable revenue stream.
With features like real-time claim scrubbing, automated billing, AI-driven denial management, and flexible patient payment options, Paynova is the ideal solution for any healthcare provider looking to maximize revenue and reduce administrative burdens.
Want to transform your medical billing process? Discover how Paynova can help you reduce denials and boost revenue today!
Frequently asked questions
1. What is Paynova Medical Billing Software?
Paynova is an advanced medical billing software that helps healthcare providers manage claims, reduce denials, and speed up reimbursements.
2. How does Paynova reduce claim denials?
Paynova checks claims for errors, verifies insurance details in real time, and ensures all required documents are attached before submission. This reduces the chances of claim rejections.
3. Can Paynova integrate with my existing EHR system?
Yes, Paynova seamlessly integrates with Electronic Health Records (EHR) and Practice Management Systems (PMS) to streamline billing and reduce manual data entry.
4. Does Paynova support multiple insurance providers?
Yes, Paynova works with multiple insurance payers and supports claims for Medicare, Medicaid, and private insurers.
5. How does Paynova help with patient payments?
Paynova offers online payment options, installment plans, and automated reminders to help patients pay their bills on time.
6. Is Paynova easy to use for small clinics?
Yes, Paynova is designed for all healthcare providers, from small clinics to large hospitals, with an easy-to-use interface and automation features.
7. Can Paynova handle recurring billing for subscription-based services?
Yes, Paynova supports automated recurring billing, making it ideal for telehealth and concierge medical services.
8. Is Paynova compliant with healthcare regulations?
Yes, Paynova follows all industry standards, including HIPAA, Medicare, and Medicaid regulations, ensuring compliance and data security.














