Behind every successful hospital or health system is a finely tuned financial engine. However, as healthcare costs climb and rules around billing and insurance get more complicated, hospitals have to find smart ways to stay financially healthy without cutting corners on care.
That’s where revenue integrity comes in. It helps teams document treatments properly, bill accurately, and get paid what they’re owed.
In this blog, we’ll break down what revenue integrity means, why it matters, and how it supports the financial strength of healthcare organizations.
Table of Contents
What Is Revenue Integrity?
Revenue integrity is the strategic process of maintaining accurate and compliant billing practices. It includes clinical documentation, coding, charge capture, billing workflows, and regulatory adherence — all working together to produce clean claims and appropriate reimbursement. It’s a cross-functional framework involving clinical, financial, and compliance teams.
Why Revenue Integrity Matters in RCM
While RCM focuses on optimizing workflows, reducing denials, and accelerating cash collection, revenue integrity safeguards the accuracy and legitimacy of revenue within that cycle.
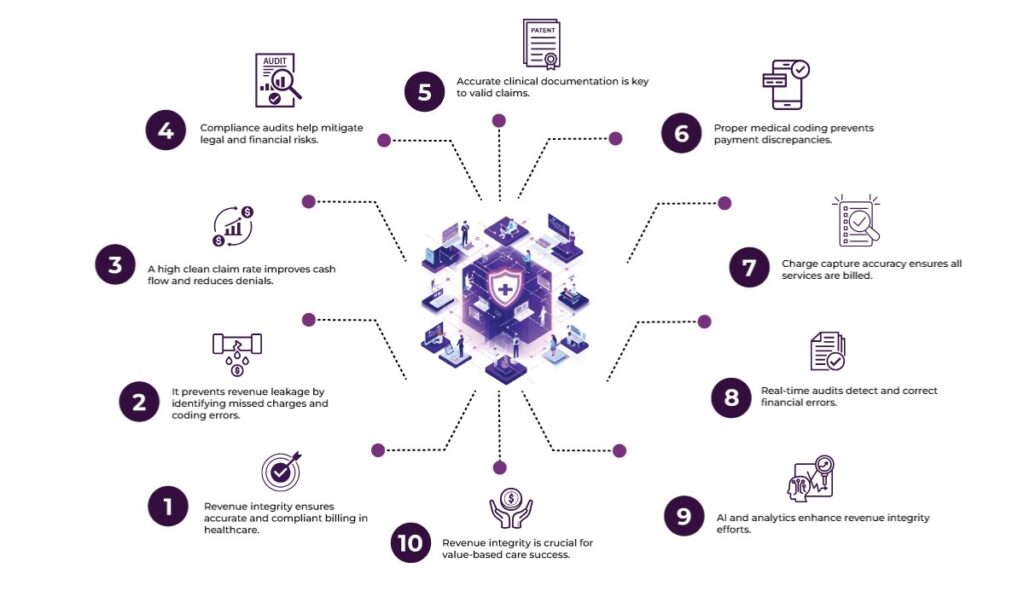
Here’s why revenue integrity is critical in making RCM more effective:
1. Minimizing Revenue Leakage
Revenue leakage is one of the most common issues plaguing healthcare organizations. It can happen due to missed charges, incorrect coding, incomplete documentation, etc. Revenue integrity programs catch these gaps before claims are submitted, which prevents underpayments or costly audits later.
By aligning clinical actions with financial records, organizations reduce the risk of money slipping through the cracks.
2. Promoting Clean Claim Rates
Clean claims — those submitted without errors and paid upon first submission — are a critical metric in RCM. A high clean claim rate shortens the revenue cycle, boosts cash flow, and reduces administrative costs.
Revenue integrity teams play a direct role in clean claim performance. They audit documentation, validate codes, and monitor claims to flag discrepancies before they hit payer systems.
3. Enhancing Compliance and Reducing Risk
Healthcare is governed by a maze of regulations, from HIPAA and CMS rules to payer-specific requirements. Revenue integrity helps organizations comply with these standards and reduces the risk of penalties or reputational damage.
It brings together coding experts, compliance officers, and auditors to monitor billing activities and implement corrective actions proactively.
The Building Blocks of Revenue Integrity
For revenue integrity to thrive, healthcare organizations need to develop systems and habits that promote transparency and accountability. Let’s explore the core components:
1. Accurate Clinical Documentation
Documentation is the basis of revenue integrity. If physicians or nurses don’t record services accurately, coders can’t assign proper codes, and billers can’t generate valid claims. Clinical documentation improvement (CDI) programs support this effort by training clinicians to document clearly and in line with coding standards.
2. Precise Medical Coding
Medical coders translate clinical encounters into CPT, ICD-10, and HCPCS codes. These codes determine what services are billed and how much providers get paid. Inaccurate coding can lead to denials, overpayments, or underpayments. Therefore, revenue integrity requires coders to stay updated on coding guidelines, changes, and payer rules.
3. Charge Capture Accuracy
Charge capture is the process of recording all billable services. Missed charges commonly cause revenue loss, especially in high-volume specialties like emergency medicine. Revenue integrity audits focus on charge capture processes to spot inconsistencies and reduce missed revenue opportunities.
4. Real-Time Auditing and Monitoring
Revenue integrity doesn’t stop once a claim is submitted. Ongoing audits of both clinical and financial records allow organizations to catch patterns, correct errors, and identify training needs. Internal monitoring also helps reduce audit exposure from payers or government agencies.
How Revenue Integrity Teams Work
Many hospitals have established dedicated revenue integrity teams at the intersection of clinical operations, finance, coding, and compliance. These teams work collaboratively to streamline processes, standardize best practices, and fix gaps in documentation or billing.
Here’s a closer look at what they typically do:
- Charge reconciliation: Matching clinical services with billed charges.
- Documentation reviews: Checking that clinical notes support billed procedures.
- Denial analysis: Investigating denied claims for root causes tied to coding or documentation.
- Technology integration: Using analytics tools to detect anomalies, underbilling, or overbilling trends.
- Education and training: Providing workshops or 1-on-1 coaching for physicians, coders, and billing staff.
The goal is to build a culture of accountability where every team understands how their work impacts the revenue cycle.
The Role of Technology in Revenue Integrity
As healthcare becomes more digital, technology is becoming a key enabler of revenue integrity. Advanced analytics, AI-powered coding tools, and revenue cycle platforms now help organizations catch issues earlier, reduce manual errors, and stay audit-ready.
1. AI-Powered Coding Assistance
AI-driven computer-assisted coding (CAC) tools can review clinical documentation and suggest the most appropriate codes. These tools enhance speed and accuracy, reduce coder burnout, and flag potential compliance issues.
2. Revenue Integrity Dashboards
Modern revenue integrity dashboards provide real-time insights into charge capture, claim status, denial trends, and coding discrepancies. Leaders can use these dashboards to make informed decisions and focus improvement efforts where needed.
3. Audit and Compliance Tools
Digital audit tools help teams conduct retrospective and prospective audits with ease. Some platforms can automatically match documentation to billed charges and identify inconsistencies for review.
Revenue Integrity in Value-Based Care
As healthcare shifts from fee-for-service to value-based care, revenue integrity will take on an even more strategic role. Under value-based models, accurate data is critical for reporting quality metrics, tracking patient outcomes, and qualifying for performance incentives.
Revenue integrity helps organizations present a clear and truthful picture of the care they deliver — not only for reimbursement but also for population health initiatives and payer negotiations.
Final Thoughts
Revenue integrity isn’t just about catching billing errors or avoiding denials — it’s about building a financially responsible, compliant, and high-performing organization. By connecting clinical documentation, coding, and billing into one cohesive strategy, healthcare providers can improve financial outcomes while staying focused on what truly matters: patient care.
At Helixbeat, our expert-led solutions can help you build a smarter, more efficient revenue cycle — one that drives both financial and clinical success. Connect with us today to get started.
FAQs
1. What does revenue integrity mean in healthcare?
Revenue integrity refers to the coordinated approach of maintaining accurate documentation, proper coding, correct billing, and compliance with regulations to generate clean claims and receive appropriate reimbursement.
2. How does revenue integrity support the revenue cycle management (RCM) process?
It complements RCM by focusing on the accuracy of the revenue flowing through the cycle. While RCM manages the process of getting paid, revenue integrity protects the quality and legitimacy of those payments.
3. How is revenue integrity evolving under value-based care models?
In value-based care, revenue integrity helps healthcare providers track outcomes, document quality, and report accurate data to qualify for performance-based payments and incentives.
4. How does accurate documentation influence revenue integrity?
Precise clinical documentation allows coders to assign correct codes and billers to submit valid claims. Without it, errors can lead to denials or revenue loss.
5. Who typically makes up a revenue integrity team?
These teams are usually composed of clinical staff, coding professionals, billing experts, and compliance officers working together to align clinical and financial workflows.














